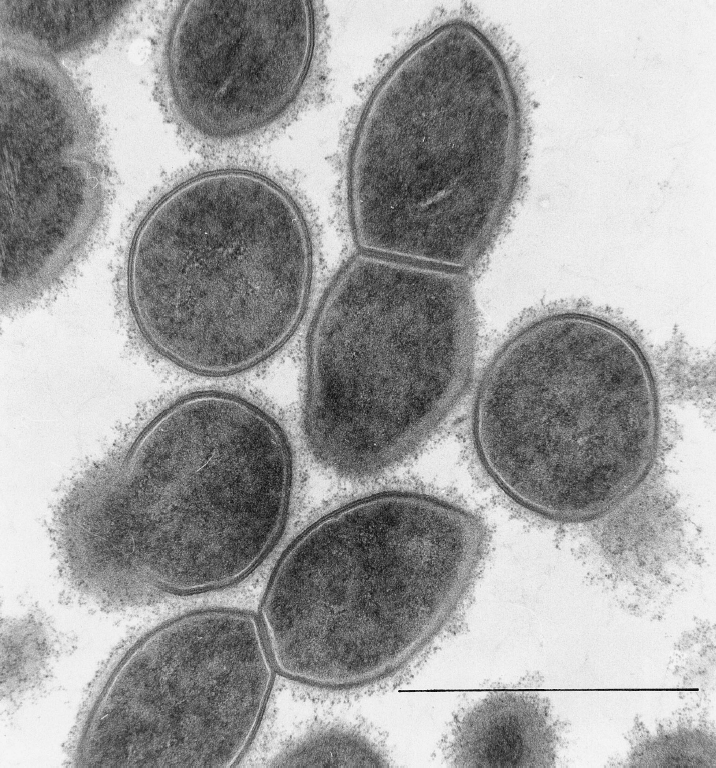
Streptococcus pneumoniaeOverview: Streptococcus pneumoniae is a Gram-positive, non-spore-forming, non-motile, lancet-shaped coccus anaerobe and a member of the Streptococcaceae family of bacteria (Figure 1). This organism has a capsule comprised of peptidoglycan and teichoic acid that protecting it from complement C3b opsonization, and is alpha-hemolytic. Choline residues that make-up teichoic acid lipoteichoic acid found on the cell wall allow the bacterium to adhere to choline-binding receptors on human cells. Choline-binding receptors are located on cells found throughout the whole body, thus permitting S. pneumoniae bacteria to effortlessly enter targeted areas. Individual bacteria are between 0.5 and 1.25 µm (micrometres) in diameter, and are found normally in the upper respiratory tract, including the throat and nasal passages. They are mesophillic, living optimally at temperatures between 30°C and 35°C.
Figure 1. An electron micrograph of nonencapsulated Streptococcus pneumoniae bacteria [Bar: 1 mm]. The difference between S. pneumoniae and other species of the Streptococcus genus is that they lack catalase and M protein. This pathogen also ferments glucose to lactic acid, and chemically hydrolyzes insulin. S. pneumoniae genome is a closed circular DNA containing 2 to 2.1 million base pairs. Colonization occurs when the pathogen engages with the host, proliferates, and attempts to invade the lower airways. When this occurs, the host deploys innate, cell-mediated, and humoral defense mechanisms to prevent the pathogen from entering past tissue barriers. If colonization is successful, it will be carried throughout the nasopharynx for up to four to six weeks. Virulence: The pathogenicity of S. pneumoniae has been attributed to various structures, most of which are situated on its surface. S. pneumoniae contains more than 500 different surface proteins. A notable group is the family of choline-binding proteins, and among these proteins are found important determinants of virulance, including pneumococcal surface protein (PspA), autolysins (LytA, LytB, and LytC), and adhesin (CbpA). Other factors, including cell wall components and the intracellular toxin pneumolysin, are involved mainly in the inflammation caused by infection. The inflammation process probably fully develops only after lysis of bacteria by autolysin. Since inflammation is thought to induce most of the symptoms of pneumococcal disease, this group of virulence factors may thus be more directly responsible for the morbidity and mortality caused by this pathogen once bacteria have infected the host. (AlonsoDeVelasco et al., 1995). Since the amount of hydrogen peroxide produced by S. pneumoniae is similar to that produced by activated neutrophils, this oxidant might be involved in the pathogenesis of this organism by causing lung injury. Mechanism of Virulence: The capsule works by preventing the activation of the alternative complement pathway and by resisting phagocytosis. The cell wall, not to be confused with capsule, plays a role in inflammation; it activates the alternative complement pathway, resulting in anaphylatoxin production. It also enhances vascular permeability, mast cell degranulation, and polymorphonuclear leukocyte activation. It induces the generation of interluekin-1 (IL-1), which is cytopathic for endothelium, and is a mediator of attachment to endothelial cells. Pneumolysins are cytolytic at high concentrations; they inhibit ciliary movement and disruption of epithelium, inhibit of bactericidal activity of polymorphonuclear leukocytes, lymphocyte proliferation, and antibody synthesis. Furthermore, autolysins produced by S. pneumoniae release pneumolysin and cell wall products, while peptide permeases enhance adhesion of the bacterium to the target cell. Finally, complement factor H-binding component inhibits complement activation and phagocytosis (AlonsoDeVelasco et al., 1995). S. pneumoniae infection can lead to the inflammation of the sinus, brain, heart, or the whole body (sepsis). It can also cause repeated ear infections (otitis media), meningitis, infection of the bone marrow, or even death, especially since there are multiple antibiotic-resistant S. pneumoniae stains. The transmission of this organism is person to person. Those most susceptible to infection are either very young, very old or are immunocompromised (people with AIDS or cancer). Persons most at increased risk are those who are present in child-care centers, old age homes and those who use antimicrobial agents. The main disease caused by S. pneumoniae is pneumonia. Pneumonia can be broken down into two forms, namely, bronchial and lobar. Bronchial pneumoniae is prevalent in infants, children, and aged adults. Lobar pneumoniae, involving a single lobe, or section, of a lung, occurs mainly in younger adults. The majority of lobar pneumonia cases are caused by Streptococcus species. One of the ongoing issues of this disease is that it occurs mainly in children less than the age of two because of their lack of immunity. The main target of study today is to accomplish making a vaccine for under the age of two to prevent life-threatening infections cause by S. pneumoniae, since it is one of the leading bacterial causes of death. References: Alonso DeVelasco, E., Verheul, A.F.M., et al. (1995). Streptococcus pneumoniae: Virulence Factors, Pathogenesis, and Vaccines. Microbiological Reviews, 59(4): 591–603. |
Alpha-hemolytic: When alpha hemolysis is present the agar under the colonies is dark and greenish. This is sometimes called green hemolysis because of the color change in the agar. Alpha hemolysis is caused by hydrogen peroxide produced by the bacterium, oxidizing hemoglobin to green methemoglobin. Compare with beta-hemolysis.
|