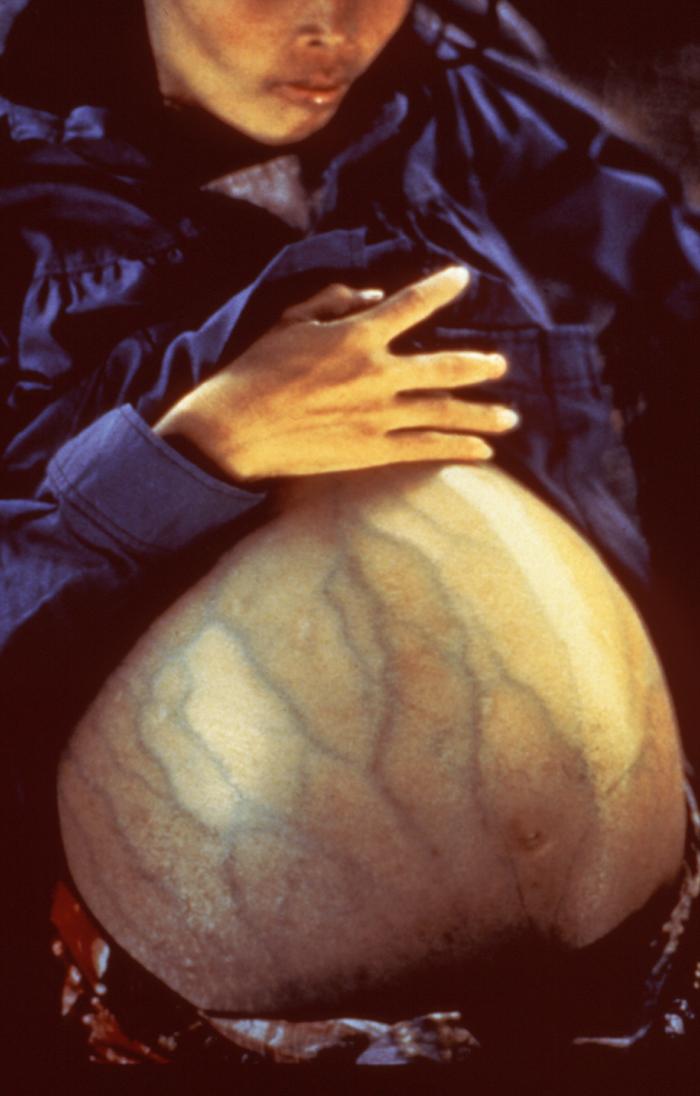
Hepatitis B VirusContents Characteristics of Infection: The virus mostly attacks liver parenchymal cells. Up to 30% of infected people show no symptoms, and symptoms are even less common in children. HBV infections are defined as acute for the first six months after exposure. A key indicator of an acute infection is the hepatitis surface antigen (HBsAg) which is found attached to the lipid membrane of the envelope. Likewise, hepatitis B (HB) virus DNA, HB c-antigen, HB s-antigen, and HB e-antigen are also detectable in the bloodstream. The term antigen refers to a component of the virus (or any pathogen), such as a particular protein it possesses, that can be detected by an antibody produced in the person's body and cause an immune response against the antigen. The term antibody refers to a complex protein produced by cells of the immune system, such as B lymphocytes (B Cells), that attach to antigens and allow for their uptake and destruction. During the acute infection, the liver produces large quantities of empty virus which travels through the bloodstream, allowing for HBsAg to be detected. If the virus goes into ‘hiding’ – or stops producing new viruses, or produces viruses at such a low rate that the surface antigen cannot be detected – the individual is said to be a carrier. HBV DNA is used to monitor the antiviral therapy of chronic patients. Chronic infections can lead to cirrhosis (scarring) of the liver, liver cancer, liver failure, and eventually death. Death occurs in 15-25% of chronically infected people due to liver complications. The virus itself does not damage the liver cells, but the immune response, mostly MHC class I CTLs attacks the cells in an attempt to kill the virus hiding within (Buendia, 1998). Hepatocellular carcinoma (type of liver cancer) is attributed to the continuous necrosis and regeneration of the cells, which increases the chances of DNA damage and mutagenesis (Figure 3). The accumulation of these alterations may lead to cancer, but there are some properties of the HBV life cycle that have been shown to have oncogenic effects. One of these would be the insertion into the genome, which increases the instability of the host genome, leading to large deletions and rearrangements (Buendia, 1998). Figure 3. This female Cambodian patient presented with a distended abdomen due to a hepatoma resulting from chronic hepatitis B infection. The incidence of hepatocellular carcinoma in patients with a hepatitis B infection is 12 to 300 times greater. The HBV DNA is incorporated into the hepatocytic DNA during the disease pathogenic process. Those who go on to develop chronic hepatitis B and fail to take any medication to treat their condition often develop jaundice, which is characterized by the yellowish staining of the skin or eyes. Jaundice is caused by an increase in blood plasma bilirubin, which is a chemical derivative of biliverdin - a chemical breakdown component of hemoglobin. Bilirubin is naturally yellow in colour, whereas biliverdin is naturally green. Increased levels of bilirubin in the blood suggests that red blood cells have been damaged and have released free hemoglobin into the bloodstream. Usually when the virus first enters the bloodstream, phagocytes such as macrophages take up the virus and release potent chemical agents to destroy the pathogen. These chemicals have an effect on neighboring cells, including red blood cells. Since blood and lymph pass through the liver, kupffer cells (specialized liver macrophages) and natural killer cells of the immune system are actively destroying free-hepatitis B virus flowing in the bloodstream and viral-infected cell, respectively, and subsequently damaging red blood cells.
|