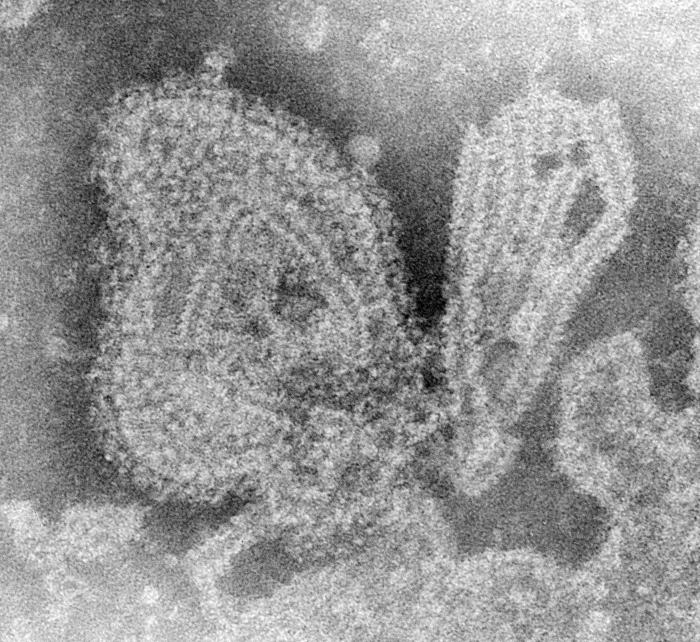
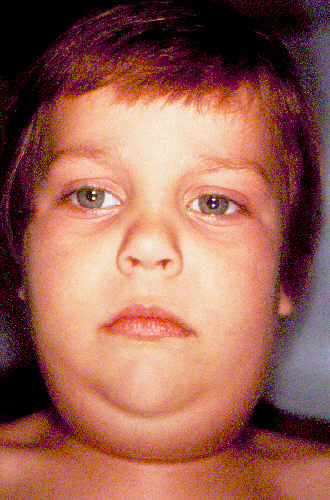
Mumps VirusOverview: Mumps virus is a single-stranded, negative-sense, enveloped RNA virus and a member of the Paramyxovirus family (Figure 1). The organism is roughly 150 nm (nanometres) to 300 nm in diameter and possesses a tube-like, helically symmetrical nucleocapsid containing a monopartite RNA genome and an RNA-directed RNA polymerase. Mumps virus causes an acute disease most common in children and young adults. It is transmitted by direct or close person-to-person contact, and school children are the main source of the spread. The pathogen is transmitted by salivary gland secretions, mainly just before and shortly after clinical onset (Baron, 1996). The only natural host of mumps virus is humans, although experiment infection has been induced in several species, most significantly, in monkeys, hamsters, mice, and rats. Figure 1. A negative stained transmission electron micrograph depicting the ultrastructural features displayed by the mumps virus. Pathogenicity: Mumps virus enters the body through the pharynx or the conjunctiva. Once it moves into the bloodstream, it is carried to various organs, namely, salivary glands, testes, ovaries, pancreas, and the brain. The virus, however, localizes in the throat. Once the pathogen becomes situated in this targeted region, viral replication takes place in the ductal cells of the glands, inducing large amounts of complimentary (minus) RNA in the infected cells. The virus gains entry into these cells using sialic acid, an acyl derivative of neuraminic acid found on cellular glycoproteins and lipids; thus, this chemical residue serves as the receptor for mumps virus. Because the mumps virus receptor is ubiquitously expressed on mammalian cells, the virus infects most cell types. Infected cells contain relatively large amounts of slowly sedimenting RNA species with genomic base sequences that function as precursors of the small RNA species found in virions. The major proteins the mumps virus encodes is NP, a protein which protects genomic RNA from cellular proteases and determines the helical structure of the capsid, P protein, which forms part of the transcriptase complex, V protein, which functions to circumvent interferon-α and interferon-γ signaling, and the F and HN glycoproteins, which are responsible for binding to host cell receptors and initiating entry. Clinical Infections: Mumps virus causes a systemic generalized infection that is spread via the bloodstream. This is followed by rapid interferon productions and specific cellular and humoral immune responses. Interferon levels will increase, thereby limiting the spread and multiplication of the virus. The amount of interferon will continue to increase until humoral antibodies and cell-mediated immunity appear, at which point interferon levels decrease (Baron, 1996). Within the first three days after the onset of symptoms, immunoglobulin M (IgM) antibodies rapidly develop and persist for two to three months. A few days later, immunoglobulin G (IgG) antibodies appear and persist for life to ensure lifelong protection again recurrent disease. The symptoms of mumps virus typically start within a few days of fever, headache, muscle aches, tiredness, and loss of appetite, and is followed by inflammation of the salivary glands (parotitis) (Figure 2). Figure 2. Child with mumps. Complications as the result of contracting mumps virus can include (1) inflammation of the brain and/or tissue covering the brain and spinal cord (encephalitis/meningitis), (2) inflammation of the ovaries (oophoritis) and/or breasts (mastitis) in females who have reached puberty, and (3) deafness. Typical cases of mumps involving the salivary glands can usually be diagnosed without laboratory tests. Identification: Acute infections can be diagnosed by isolating the virus from saliva, cerebrospinal fluid or urine in cell culture. Serologic evidence of acute infection is obtained using the Enzyme-Linked Immunosorbent Assay (ELISA) or an immunofluorescence test early after onset of symptoms by demonstrating IgM antibodies in the first serum and later by detecting a significant IgG antibody rise in paired sera. An alternative to antibody detection in serum is the detection of IgM and IgA antibody in saliva (Baron, 1996). It is also possible to detect the virus through direct reverse transcriptase polymerase chain reaction or virus isolation with sequence analysis. Mumps viral RNA may be detected from viral samples prior to onset of parotitis until five to nine days after parotitis, whereas one to four days is optimal for virus collection. This is an important method of detection among previously immunized suspected cases. Vaccination: Active vaccination of the MMR vaccine (protecting against measles, mumps, and rubella) has reduced the incidence of reported mumps and mumps complications by more than 90 percent. It is recommended for all children at 12 to 18 months of age. The mumps component contains attenuated virus grown in chick embryo tissue culture (Baron, 1996). The vaccination is given in two doses. The first dose is give between 12 to 14 months of age and the second dose is given at either 6 or 12 to 13 years of age to enhance antibody levels (Baron, 1996). There has been debate over the years as to the harmful effects of the MMR vaccine. Recently in the news, the Lancet (peer-reviewed journal) retracted the 12 year old paper that sparked an international crisis of confidence in the safety of the MMR vaccine when its lead author suggested a link between the vaccine and autism. The author of the study - Andrew Wakefield - was found guilty of:
References: Baron, S. (1996). Medical Microbiology (4th ed.). |
 that lisa simpson
(shown below), from the popular television
series the simpsons, had the mumps in season 2, episode 16.
that lisa simpson
(shown below), from the popular television
series the simpsons, had the mumps in season 2, episode 16.
|